Common Infections You Could Acquire In Hospital
Hospitals are life-saving institutions that save around 50,000 lives in the U.S. every year. However, between 35% and 70% of hospital-acquired infections (HAIs) could be prevented, according to the World Health Organization (WHO). They state that better hand hygiene and improved prevention and control practices could make hospitals safer places. So, what HAIs are you most likely to get when you’re admitted and how can hospitals prevent them?
Pneumonia (HAP)
Hospital-acquired pneumonia (HAP) occurs more than 48 hours after admission to the hospital. A study in the BMC Pulmonary Medicine found that certain treatments in hospitals can cause HAP, including mechanical ventilation and being admitted to intensive care. The study also revealed that hospital wards with six beds or more per room and a higher bed-to-nurse ratio were more likely to have patients that develop HAP. This indicates that exposure to too many patients may contribute to HAP. Overworked nurses may also be cutting corners and not hand-washing between patients. Five medical practices in the U.S. have recently announced new measures to prevent HAP which include elevating the head of the bed, providing oral care, and minimizing sedation, so hopefully cases of HAP will reduce soon.
Sepsis (HAS)

More than 23% of all cases of sepsis are acquired in hospitals. Bacterial infections typically cause sepsis, although it can also be caused by fungal, parasitic, and viral infections. These are usually the result of an infection entering the body during a medical procedure. Hospitals must improve their infection control measures to prevent their patients from developing sepsis. Hospital-acquired sepsis (HAS) is more prevalent in low-performing hospitals than in high-performing ones (22% compared to 9%). This suggests that there’s a lot more many hospitals should be doing to prevent it. Failure to do this can result in serious repercussions, including organ dysfunction, loss of limbs, mental decline, and mortality. In cases like this, medical malpractice may be to blame and legal assistance will be needed. When speaking about medical malpractice JJS Justice says “we can help hold those responsible accountable and deliver the full measure of justice you deserve.”
Clostridium Difficile Infections (C.diff)
75% of all cases of Clostridium difficile infections (C.diff) are contracted in hospitals. C.diff is transmitted by feces and is most commonly acquired in hospitals from healthcare workers touching contaminated surfaces and passing it onto patients. There is now some evidence that it’s airborne too. For this reason, isolating individuals with C.diff in hospital is highly recommended. Healthcare workers must ensure they wear gloves and an apron when treating patients with C.diff, dispose of them correctly immediately afterward, and wash their hands before seeing their next patient. Hospitals must also avoid prescribing antibiotics unless absolutely necessary. Around 30% of antibiotic prescriptions are not needed and this increases the risk of C.diff as antibiotics affect good gut bacteria.
Surgical Site Infections (SSIs)
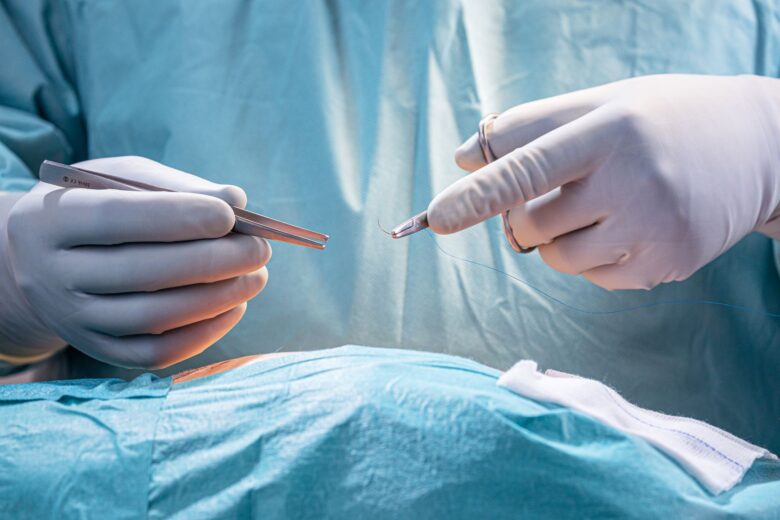
Surgical site infections (SSIs) are the second most common type of infection that people acquire in hospitals. Up to 4% of patients who have surgery get an SSI. SSIs are usually caused by instruments that aren’t sterile, poor cleaning of wounds, and inadequate stitches. These all increase the chance of microorganisms getting into the wound and infecting patients. To stop patients from getting SSIs, hospitals must prioritize health and safety. One study found that patients are more likely to get an SSI when they’ve been in hospital for 24 hours or longer. This is because of the number of bacteria they’re exposed to on hospital wards. To prevent SSIs, hospitals must thoroughly wash patients before surgery as this reduces the number of microorganisms present on their skin. Tissue damage should also be kept to a minimum as this lowers the likelihood of microorganisms getting into the wound.
Urinary Tract Infections (UTIs)
75% of people who get a UTI during a hospital stay have been catheterized, according to the Centers for Disease Control and Prevention (CDC). The longer a catheter is used, the more bacteria grows and this increases the chances of getting a UTI. One study found that after three days of a catheter being inserted, 15% got a UTI. After eight days this increased to 68%. Despite nurses being authorized to remove catheters when they see fit, they typically rely on physicians to tell them when to remove them. Studies have also found that physicians are forgetting to review whether a catheter is still required during ward rounds, clinicians are failing to communicate with each other, and catheters are being hidden under clothing and being forgotten about. Simply improving communication, fully assessing patients, and setting up a reminder system could significantly decrease the number of patients that get a hospital-acquired UTI.
Central Line-associated Bloodstream Infections (CLABSI)
It’s estimated that 250,000 central line-associated bloodstream infections (CLABSI) occur in hospitals each year. This type of infection happens when bacteria or viruses enter a patient’s bloodstream through the central line. Patients in intensive care units (ICU) are more likely to get a CLABSI. Getting a CLABSI is serious as it could mean a patient has to have their central line removed. This affects their health as it means essential medications and fluids cannot be administered. Patients with CLABSI may also experience organ damage, blood clotting issues, septic shock, or lose their lives. Mortality rates for CLABSI are as high as 25%, so hospitals must do all they can to reduce the chance of their patients developing such an infection. Strict hygiene measures should be in place. These measures should include using all five sterile barrier precautions, using antiseptic on the skin before putting the line in, using ultrasound guidance to ensure correct placement, and using the subclavian vein rather than the femoral vein. An assessment should be done daily to check whether the central line is still required. As soon as it’s no longer needed, it should be removed.
Hospitals need to take patient safety seriously. While there are some that are good at this, it’s clear to see that more can be done to prevent patients from contracting HAIs that could impact them for life.